Once I had passed the halfway
mark on my 2200nm solo sailing trip to Tubuai earlier this year and everything
had progressed smoothly to that point, numbers of people congratulated me as if
I had already arrived and suggested from there on it would be a piece of cake,
plain sailing, all downhill, no sweat….But of course then the wind went round
to the wrong quarter, and strengthened, and the seas developed into something
quite wild and so the last week turned out to be the toughest week I had ever endured sailing.
Something similar seems to be
happening here, as my last week begins, and the event I had been dreading since
arrival, the thing I am here above all to try and prevent - maternal death -
finally happened. To be honest at times Ive felt lucky that it hadn’t already
happened - Ive felt like a lone and inexperienced goal keeper leaping this way
and that to keep out a furious barrage
of attacks, but that it was only a matter
of time before one would get through. Never-the-less as the last week approached
I started to hope that maybe on my watch, none would – but that all changed
yesterday: a mother died ; her name was Erteban, she was only 23.
I wrote early in my stay here
about Etewa who arrived looking dead, with a dead baby stuck in a “Brow” presentation.
We performed a so called “destructive delivery” on that baby, using an
instrument to penetrate its skull so that its contents would be expelled and
the head collapse making vaginal delivery possible. Erteban arrived looking as
dead as Etewa did, with no recordable Blood Pressure, semi conscious,
dehydrated and the babies head stuck in
the birth canal. It was dead. We found out that she already had a healthy
toddler and this was her second pregnancy, that she hadn’t had any antenatal
care and had been in labour at home and had been trying to push the baby out
for six hours . Then her pains all stopped but by then it was midnight . In the morning they carried her for four hours
to a road and caught a bus to Motta and she arrived just after lunch. As is
typical here, she had on a horrendously filthy dress, her arms and legs looked
as if they hadn’t seen water for months, her feet were dry and cracked with
souls that were as thick and hard as a layer of bark on a tree, and she could
barely lift her head up. One valuable but ominous sign that Ive learned to recognize, is that in someone
who has previously had one or more babies , if contractions stop after thay
have been in strong labour for a long time, and now the baby is dead, it
probably means the uterus has ruptured. And when that happens there is a
massive internal bleeding. It seemed very likely that this was what had
happened. So, whereas for Etewa major abdominal surgery was avoided by the
destructive delivery, Erteban was going to need it, even though she was in
shock and desperately ill. Without surgery she would soon die from ongoing
internal bleeding, and infection carried
into the abdominal cavity by the baby expelled ther from the birth canal.-but
the operation by itself could kill her – but it was her only hope.
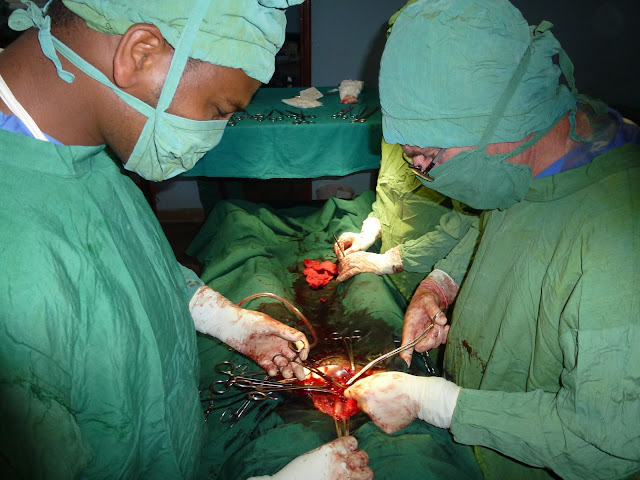
We took her to theater and it
took an hour and a half to deliver the dead baby – quite a large baby for a
small Ethiopian woman – and to repair a
huge tear in the side of the uterus. We guessed she had lost close to two
litres of blood. At the end of the procedure it was still not possible to
record her blood pressure, her pulse was racing at about 150 beats per minute, her breathing was still fast and
shallow but there was urine in her catheter, the only reassuring sign. We
tested all six of her accompanying family members to find someone with
compatible blood, but were unsuccessful, and she was too unwell for transfer to
Bahar Dar where there is a blood bank.. We were doing all we possibly could,
which was not very much.
I couldn’t imagine how she would
even survive the night, but she did. In the morning she was still desperately
unwell, but blood pressure could be recorded, she spoke a few words, and her
temperature was normal. On the other hand her pulse remained close to 150 and
her breathing was very fast. She struggled on all day as we watched for some
sign of improvement but it took hours for our one daily set of limited blood
tests to come back, and the X-Ray machine has now been unfixed for eight
months, so it was impossible to see if she had heart failure or pneumonia – so
I treated her for both. In fact nothing we did seemed to make much difference
and her condition worsened with a rising temperature, increasing restless ness
and then unconsciousness. Infection was setting in. Late on the second day,
when it was clear she would not survive the night, her grieving brothers and
husband decided they would like to take her home. Tears ran silently down their
faces as we removed the catheter and the IV lines that had given her the fluids
and antibiotics and other medicine that had prolonged her survival to that
moment, but now there was no denying it, it was too late for her. Hopefully she
would survive the road trip and being carried in the middle of the cold night
along that four hour track to her village, where the rest of the family could
comfort her for however many hours remained. It was moving to see how much they
all loved and cared for her, and how dignified and how true was their conduct.
It seemed worse to me that these poor ragged farmers who already had almost
nothing should have even their young mothers and babies taken from them.
Strangely I felt more numb than sad, and I thought about everything I had done
and wondered if there was something I
could have done differently. In fact numerous things suggested themselves to
me, and there are some things I would do differently next time, though I am not
certain the outcome would have been different . However I do know that if they
had made that four hour trek to the road at the beginning of her labour rather
than at the end, it would have been: but how were they to know? Mother nature can sometimes be a very cruel
midwife.